What is CHAOS?
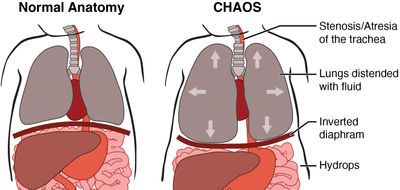
CHAOS, or Congenital High Airway Obstruction Syndrome is a blockage of the fetus’s trachea (windpipe) or larynx (voice box). This obstruction can be due to a number of factors including narrowing of the airway (stenosis), a web-like membrane, or even an area of the trachea that is missing (atresia). While in the uterus the fetal lungs constantly produce fluid. As a result of this airway blockage in the trachea, the lung fluid cannot escape out of the fetal mouth. Because of this the fetus’s lungs become distended with fluid. Overdistention of the lungs can put pressure on the heart and effect the heart’s ability to function. If the heart cannot beat effectively hydrops (congestive heart failure) can occur.
The cause of CHAOS is currently unknown. It is a very rare condition and not thought to recur in families.
What is the outcome for a fetus with CHAOS?
The outcome for a fetus with CHAOS depends greatly upon the type of malformation causing the obstruction. If the obstruction is minor, such as a thin tissue membrane covering the larynx, it may be correctable through minimal surgery before or after birth with no lasting complications. A complete blockage of the larynx, or a missing section of trachea is more serious. Babies born with this problem will not be able to breathe when they are born; as a result, require placement of a tracheostomy (breathing tube through the neck) after birth. Also multiple operations to correct the airway will be required after birth. There may also be problems with normal voice functioning, the ability to talk, or the ability to eat/drink by mouth. In more extreme cases of CHAOS where the lung swelling endangers the heart function, surgery before birth may be a treatment option.
The condition can also be complicated by the presence of other birth defects; thus, it is important to test for other abnormalities. These are done by testing the chromosomes of the fetus through amniocentesis and microarray, and also performing a cardiac echo to look more closely at the fetal heart structure and function.
How serious is fetus's condition?
CHAOS is often a very serious and life-threatening condition. The severity depends partly on whether the blockage is complete. When the blockage is complete, the lungs can become hugely overdistended and can lead to hydrops fetalis (congestive heart failure); In order to determine the severity of the problem a number of tests are recommended.
Accurate assessment requires four tests:
- amniocentesis and/or microarray to assess the fetal chromosomes
- a level II ultrasound to look for other anomalies and define the anatomy of the airway
- a fetal echocardiogram to determine whether or not the fetus has an associated heart defect or if the function of the heart has been affected
- an MRI to obtain an accurate picture of the airway and determine the level and length of the obstruction in the airway
If the chromosomes are normal, and there are no additional birth defects other than the CHAOS, the severity of the condition depends on the type of malformation causing the airway obstruction.
What are my choices during this pregnancy?
After your fetus’s condition is fully diagnosed through a formal evaluation, you will be presented with treatment options. In severe cases, where the fetus has hydrops (heart failure), surgery before birth to relieve the obstruction may be offered. Hydrops in the fetus is defined as the build up of excess fluid in the fetus. This extra fluid can be seen in the fetal abdomen, lungs, skin or scalp.
If there is no fetal hydrops, we recommend your delivery will be scheduled via EXIT (Ex Utero Intrapartum Treatment) procedure. The EXIT Procedure is used in situations in which there is a known airway obstruction in the baby. The goal of the procedure is to deliver the baby in a controlled situation so that they are not deprived of oxygen, to minimize the chance of damage to the brain of the baby.
EXIT Procedure
The goal with the EXIT procedure is to provide the baby with a functioning airway so that adequate oxygen can be delivered to the lungs after the baby is separated from placenta. The EXIT procedure is a planned, specialized delivery involving both the mother and the baby. It should only be performed at a hospital that has a team consisting of a pediatric surgeon, obstetrician, anesthesiologist, and neonatologist.The start of the procedure is conducted like a Cesarean section. However, unlike a Cesarean, the mother is put under general anesthesia in order to ensure that the uterus is completely relaxed.
The head of baby is delivered but the baby remains attached to the placenta. A pediatric surgeon uses a bronchoscope through the baby’s mouth to look more closely at the airway. Depending on the type of blockage the surgeon may then attempt to pass an endotracheal tube (tube through the baby’s mouth into the trachea) and give breaths to the baby. If this is successful, and oxygen is being delivered to the baby through the tube, the infant is delivered and the umbilical cord cut. If a tube cannot be passed from the mouth through the obstruction, the pediatric surgeon will need to place a tracheostomy tube through the neck directly into the trachea, bypassing the blockage. The surgeon will make an incision in the neck of the baby and place a tube below the level of the airway blockage. Once the tube is placed, and the surgeon is confident that it is functioning and can be used to deliver oxygen to the baby, the infant is delivered. Care of the infant is then provided by the Intensive Care Nursery team.
What will happen after birth?
To provide a functioning airway your baby will likely be delivered via an EXIT procedure. After which, your baby will be brought to the Intensive Care Nursery for close observation and further assessment. Additional reconstructive surgeries may be required.